Projects: Collaborate.Health
Telehealth to Increase Health Care Access in Underserved Communities
Increasing physician participation in telehealth programs to increase access to health care in rural and underserved communities.
- Agency Partner
- Northeast Telehealth Resource Center
- Course
- Communication Strategies for Public Health
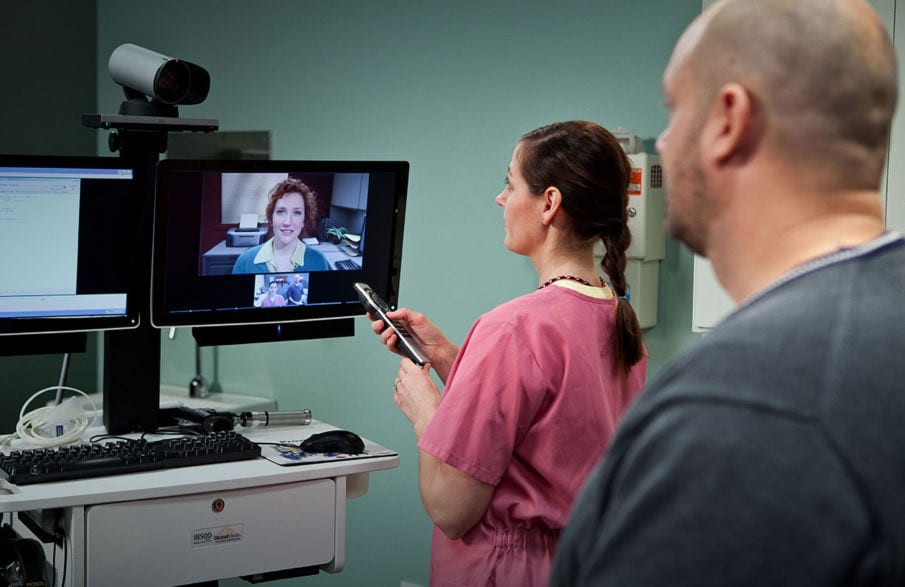
Overview
This project sought to increase physician awareness, interest, and willingness to participate in telehealth programs through quick yet informative online modules and tutorials in an effort to increase access to health care in rural and other underserved communities.
Context
Telehealth is the collection of means or methods, not a specific clinical service or medical specialty, for enhancing health care, public health, and health education delivery and support using telecommunications technologies. According to a 2016 Telemedicine Study by HIMSS Analytics, 61 percent of health care institutions, including 40 to 50 percent of all hospitals in the United States, employ some form of telehealth. Telehealth services can provide patients, providers, and health care organizations a number of benefits including increased and timelier patient access to providers, improved continuity of care, cost containment or savings, reductions in the use of institutional care, and increased patient satisfaction. Despite these benefits, a number of challenges continue to hinder health care organizations from adopting telehealth technologies including the need for training and workforce development.
The Northeast Telehealth Resource Center (NETRC) has a mission to increase access to quality health care services for rural and medically underserved populations. NETRC is federally funded to provide free, individualized technical assistance, education, and other resources to health care organizations in New England, New York, and New Jersey. NETRC works to address the challenges to telehealth adoption and implementation including increasing the awareness among consumers of the opportunities telehealth may provide, as well as the awareness, interest, willingness, and capacity of health care professionals, most notably physicians, to integrate these new services. They do this through providing short and long term technical assistance and access to educational materials to health care providers, administrators, payers, policy makers, and others.
Challenge
Increasing physician awareness, interest, and willingness to participate in telehealth programs and provide programs that are quick and informative resulting in increased access to health care in rural and other underserved communities.
Solution
The proposed intervention addressed provider engagement and implementation of telehealth in their practices and focused on increasing knowledge of telehealth and overcoming barriers to use. Several key informant interviews were conducted with providers to tailor the resulting intervention materials and components.
Results
Students redesigned a mock-up of the existing NETRC website, outline and flow of four online modules for providers, videos to demonstrate various aspects of telehealth to providers, texting applications, and tutorials on talking with patients about telehealth. Each component was short (5-10 minutes) and allowed for providers to pause and come back to the component. Students conducted a one-hour national webinar on provider access to and need for telehealth during the semester attended by over 100 domestic and global providers and administrators. One student continued with the partner organization after the semester as an intern to adapt and implement the program in other healthcare organizations.
Project Timeline
This project took six months to complete from kick-off meeting to presentation of final deliverables. Click the button below for a detailed timeline.
View Project Timeline
Student Spotlight
Meaghan Wostbrock
Meaghan received her MPH from the Boston University School of Public Health with a concentration in Social and Behavioral Sciences in 2017. Meaghan was on the NETRC Telecommunications team for SB806 – Communication Strategies for Public Health.
Throughout her MPH studies, Meaghan focused on strategic health communications as well as intervention design and program evaluation. She also worked in the BUSPH Department of Community Health Sciences and provided administrative and research support to the department’s faculty. Currently, she is a Program Specialist for a cancer research program at Weill Cornell Medicine in New York City. The program aims to establish new approaches for treating prostate cancer to improve patient survival and quality of life. Throughout her career, Meaghan has been interested in driving social change and promoting health initiatives that increase patient access to providers and resources in order to improve health outcomes.